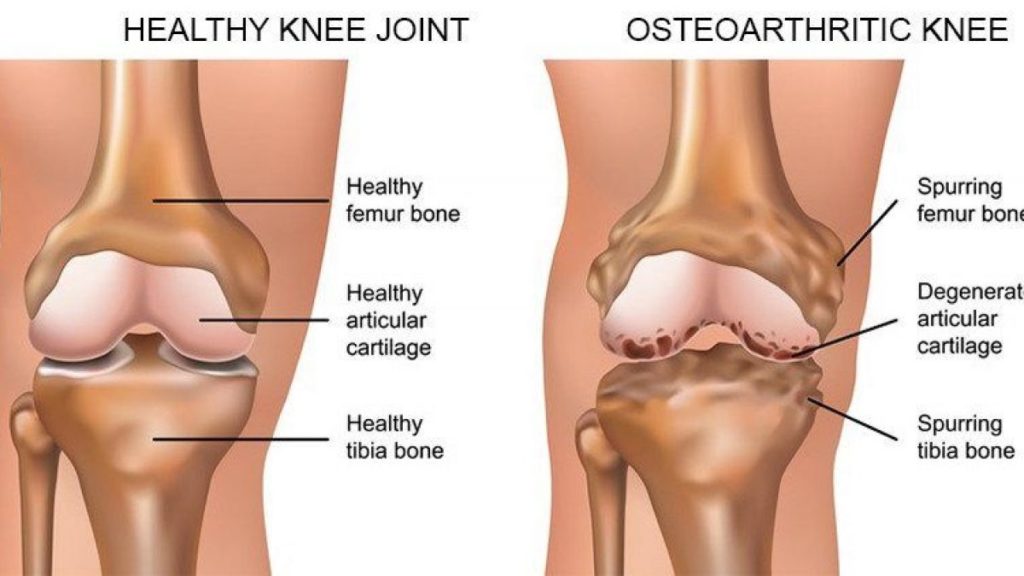
 Did you know that the knee is the largest joint in the human body? Did you also know that it is the one most likely to develop osteoarthritis? If you experience knee pain and stiffness as a result of osteoarthritis, you might benefit from understanding how the condition starts and develops within the joint over time. The following will show you how the knee’s bones, cartilage, and other soft tissues slowly change with osteoarthritis.
Did you know that the knee is the largest joint in the human body? Did you also know that it is the one most likely to develop osteoarthritis? If you experience knee pain and stiffness as a result of osteoarthritis, you might benefit from understanding how the condition starts and develops within the joint over time. The following will show you how the knee’s bones, cartilage, and other soft tissues slowly change with osteoarthritis.
What is Knee Oosteoarthritis?
Knee osteoarthritis is a condition that causes the breakdown of the cartilage and other tissues in the knee. As the condition develops and worsen, millions of people affected by it experience pain, swelling, and new or worsening inflammation. Your knee joint is positioned where your femur meets your tibia. The patella, or kneecap, glides on a groove that is at the bottom of your femur. Your fibula, a small but long bone, positioned next to your tibia is not a part of your knee joint. In the past, knee osteoarthritis was believed to be the result of an old injury or accumulative wear and tear on the joint. Today’s research has proven that low-grade inflammation throughout the human body, along with joint biochemistry, and other factors can cause knee osteoarthritis.
When the Cartilage in Your Knee Begins to Break Down
The condyles are the large, rounded parts of bone positioned at the top of the tibia and bottom of the femur. When you bend your knee, the condyles rub against each other.
There are two types of cartilage in this area…
- Meniscal Cartilage is a thick piece of cartilage that is layered between the tibia and femur. Its job is to act as the knee’s shock absorber.
- Articular Cartilage is smooth, slippery, but strong soft tissue that covers the end of your condyles. Its job is to help minimize friction when you bend and straighten your knee.
A layer of articular cartilage also exists under your knee cap and helps it glide smoothly along the front portion of your femur. One of the first signs of knee osteoarthritis is damage to the knee’s articular cartilage. The meniscus is not like articular cartilage as damage to the meniscal cartilage is its own condition separate from knee osteoarthritis, however the two conditions are intertwined.
Changes to the Knee’s Bones
When changes happen to the articular cartilage and other soft tissues, other bones in the joint begin to change as well. Such changes can be seen on x-rays and other medical imaging. A few changes can be described as follows…
- Subchondral Bone Sclerosis occurs when the surfaces beneath the tibia and femur that are under the knee cartilage change in composition and become harder.
- Osteophytes (bone spurs) are growths that might develop at the knee joint. The spurs are painless but they can cause excessive friction at the knee joint which might lead to painful inflammation.
- Bone Lesions and Cysts – when the bone develops cysts or areas of unusual swelling, it is called bone marrow lesions. These typically lead to pain in the knee.
The knee joint can experience its own changes. The synovial membrane, a delicate membrane that surrounds the arthritic knee joint, can become inflamed. As a result, those experienced it might have knee pain, swelling, and stiffness.
Joint Degeneration Worsens Without Treatment
Early signs of knee osteoarthritis are stiffness and aching pain in your knee. If left untreated, the condition will most likely get worse leading to the disappearance of thinning knee cartilage. Fortunately, there are several treatments that may slow down or stop the progression of knee osteoarthritis. Your healthcare practitioner can assist you in finding the treatment options that will work best for you based upon how bad you osteoarthritis is developing, in addition to your health and lifestyle.
You May Not Experience Symptoms with Arthritis
Knee pain is not always the tell-tell sign of osteoarthritis. In some instances, doctors have discovered mild joint degeneration on a person’s x-rays without them feeling pain or symptoms. Osteoarthritis symptoms can be unpredictable making it hard to assume that all knee pain is the result of knee osteoarthritis. You can have bone on bone osteoarthritis with mild or now symptoms. It is not clear why such differences exist but they do. This makes it harder for you to pinpoint your issues and get help with them immediately.
For persistent pain that is interfering with your daily activities, see a rheumatologist to make the correct diagnosis and begin the proper treatment.
Contact Us (859-331-3100) For More Information to Request an Appointment
—
 About Tristate Arthritis and Rheumatology
About Tristate Arthritis and Rheumatology
Tristate Arthritis and Rheumatology is first and largest Rheumatology practice in the Northern Kentucky area. Founded by Dr. Arthur Kunath in 1986, our rheumatology practice now consists of six doctors who are board certified in both Internal Medicine and Rheumatology and a Physician Assistant. Patients see one doctor (except in emergencies), thereby assuring continuity of care and an individualized doctor-patient atmosphere giving the physician the ability to establish personalized and detailed relationships. Our doctors have received numerous awards, including being listed as “Top Doctors” in Cincinnati Magazine, receiving the Patient’s Choice Award, the Most Compassionate Doctor Award, and the American College of Rheumatology’s “My Doc Rocks” award.
>> Learn More